
Sacroiliac (SI) joint disorders are a challenging condition affecting up to 30 percent of patients with chronic lower back pain. According to published scientific data, it is common for pain from the SI joint to feel like disc or lower back pain. For this reason, SI joint disorders should always be considered in lower back pain diagnosis.
Anatomy of the SI Joint
The SI joint is located in the pelvis; it links the iliac bones (pelvis) to the sacrum (lowest part of the spine above the tailbone). It is an essential component for shock absorption to prevent impact forces from reaching the spine.
The SI joint is the function of the triangular-shaped sacrum and the pelvis. Structurally and mechanically, it is like a keystone that connects the torso to the pelvic ring/arch and legs.
The joints have limited mobility, but like any joint, may be susceptible to arthritic changes over time, especially in patients who have had prior lumbar fusions.
Lower Back Pain and the SI Joint
The SI joint is a significant cause of lower back pain and may affect populations in all age groups. It may be due to direct trauma, a fall, a motor vehicle accident, or childbirth. Clinical publications have identified the SI joint as a pain generator in 15-30 percent of chronic lower back pain patients. In addition, the SI joint is a pain generator in up to 43 percent of patients with continued or new-onset lower back pain after lumbar fusion.
Like any other joint in the body, the SI joint can degenerate or its supporting ligaments may be injured. When this happens, people can feel pain in their buttocks, lower back, groin, and even their legs. This is especially true with lifting, running, walking, or lying on the involved site.
It is important to note that on occasion, patients who have not had symptomatic relief from lumbar spine surgery may actually have had other issues to begin with. Pain in the lower back and buttocks may come from the SI joint, the hip, the spine, or any combination of these three interrelated potential pain generators.
SI Joint Dysfunction
Pain from SI joint dysfunction can be felt anywhere in the lower back, buttocks, or in the legs. Chronic SI joint pain or dysfunction can make it difficult to perform common daily tasks and can affect many aspects of a patient’s life.
Do you have SI Joint pain?
Symptoms of SI Joint Disorders
Pain is often in the buttocks with radiation into the thigh or groin but can also be present in the low back. The following are typical symptoms of SI joint disorders:
- Lower back pain
- Pain, numbness, tingling, and weakness in lower extremity
- Pelvis/buttock pain
- Hip/groin pain
- Feeling of leg instability (buckling, giving way)
- Disturbed sleep patterns due to pain
- Disturbed sitting patterns (unable to sit for long periods, sitting on one side)
- Painful sitting
- Painful sit-to-stand
- Painful climbing stairs
Causes of SI Joint Pain
Many people have pain that worsens over time; however, over half the time, SI joint pain can be related to a specific event, often an injury. It is difficult to relate any single specific functional difficulty (including walking, sitting, standing, sleeping on the affected side, job activity, bowel movements, cough, sneeze, etc.) directly to the SI joint as a source of pain.
Other causes may be due to
- Trauma to the Lumbar Spine or Hips
- Prior Lumbar Fusion
- Pregnancy/Childbirth
- Inflammatory Joint Disease (e.g. Sacroiliitis)
- Degeneration Due to Age
- Leg Length Discrepancy
Diagnosing SI Joint-Related Problems
Dr. Ball will consider all the information you provide, including any history of injury, location of your pain, and problems standing or sleeping. As part of your physical exam, he will ask you to stand or move in different directions and point to where you feel pain, and he may feel for tenderness over your SI joint.
A variety of tests performed during the physical examination may help reveal the SI joint as the cause of your symptoms. Sometimes, X-rays, CT-scan, or MRI may be helpful in the diagnosis of SI joint-related problems. It is also important to remember that more than one condition (like a disc problem) can coexist with SI joint disorders.
The most relied upon and accurate method to determine whether the SI joint is the cause of your lower back pain symptoms is to inject the SI joint with a local anesthetic. The injection is delivered with either fluoroscopy or CT guidance to verify the accurate placement of the needle in the SI joint. If your symptoms are decreased by at least 50 percent, it is likely that the SI joint is either the source of or a major contributor to your lower back pain. If your symptoms do not improve after SI joint injection, it is less likely that a problem with your SI joint is the cause of your lower back symptoms.
Treatment Options
Once the SI joint is confirmed as the cause of your symptoms, treatment can begin. Some patients respond to physical therapy, the use of oral medications, or injection therapy. The anti-inflammatory effect of SI joint injections is not permanent and does not stabilize the SI joint.
Intermittent use of a pelvic belt may provide symptom relief as well. Treatments such as injections or use of a belt are performed repetitively and symptom improvement using these therapies may be temporary. When conservative methods fail, minimally invasive SI joint fusion may be performed on an outpatient basis or with a 23 hour overnight stay at the hospital or surgery center.
SI Joint Fusion with the iFuse Implant System®
The only fusion option approved by Medicare due to its excellent clinical outcomes and longevity of use is the iFuse Implant System manufactured by SI-BONE, Inc. This is a minimally invasive surgical SI joint treatment option that provides stabilization and fusion of the SI joint for some causes of SI joint pain. This is accomplished by inserting triangular-shaped titanium implants across the sacroiliac joint to maximize post-surgical stability and weight-bearing capacity. The procedure is done through a small incision over the buttock and takes about an hour
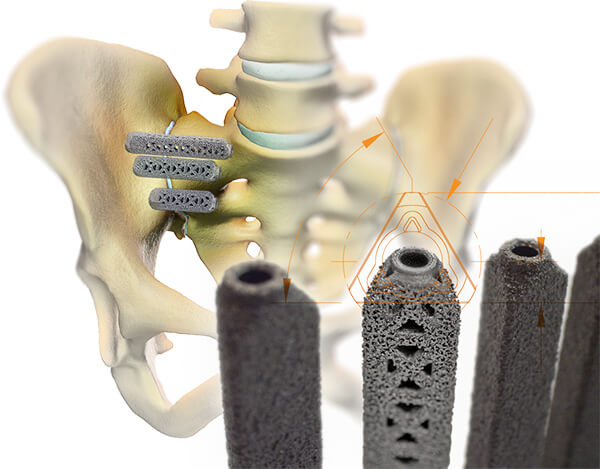
SI joint treatment using the patented triangular design of the iFuse ImplantTM has produced unparalleled clinical results. More than thirty published, peer-reviewed articles demonstrate the safety and effectiveness of the iFuse Implant System. iFuse is the only SI joint fusion system with clinical studies demonstrating that treatment improved pain, patient function, and quality of life.
SI Joint Problem and SI Fusion Surgery FAQS
Who is at risk for SI joint problems?
Women may be at increased risk for SI joint problems because of their broader pelvises, and greater curvature of the lumbar spine, which result in different SI joint biomechanics. Women also have more elastin in the collagen that makes up their ligaments. Elastin is a molecule that allows increased flexibility of ligaments. In addition, pregnancy often results in stretching of the sacroiliac ligaments. Some women have permanent changes to the SI joint ligaments as a result of pregnancy and vaginal childbirth.
How would you know that your SI joint is not functioning properly?
If you have trouble sleeping comfortably, or frequently experience your leg giving way, pain in certain lying or bending positions, or tenderness in your buttocks, you may have an SI joint disorder.
How easy is it to diagnose SI joint problems?
It is not always easy to diagnose SI joint disorders, but provocative tests and injections are helpful for confirming the SI joint as the pain source. Sometimes your physical findings indicate a SI joint condition, but chronic changes may also be seen in your lumbar spine.
Who is a good candidate for the SI joint fusion surgery with the iFuse Implant System?
The iFuse Implant System (“iFuse”) is intended for sacroiliac joint fusion for conditions including sacroiliac joint dysfunction that is a direct result of sacroiliac joint disruptions and degenerative sacroiliitis. This includes conditions whose symptoms began during pregnancy or in the peripartum period and have persisted postpartum for more than 6 months.
Are there any before surgery instructions to follow for SI joint fusion surgery with iFuse Implants?
You will be told when to stop eating and drinking before surgery. If you take a daily medication, ask if you should still take it the morning of the surgery. It is critical to inform Dr. Ball if you are taking any blood-thinning medication. At the hospital, your temperature, pulse, breathing, and blood pressure will be checked. An IV (intravenous) line may be started to provide fluids and medications needed during surgery.
What can you expect during your SI joint fusion surgery with iFuse Implants?
The SI joint fusion is performed in an operating room with either general or spinal anesthesia. You will be lying face down while your surgeon uses a specially designed system to guide the instruments that prepare the bone and insert the implants. Both the surgical technique and the iFuse Implant System are designed to offer maximum protection to your surrounding tissues.
The entire procedure is performed through a small incision, approximately 2-3 inches long, along the side of your buttock. During the procedure, fluoroscopy provides your surgeon with live imaging to enable proper placement of the implants. Normally, three implants are used, depending on your size.
The procedure takes approximately 1 hour. You may feel comfortable enough to return home the same day of surgery or perhaps the morning after. Dr. Ball will make this decision based on your post-surgical status.
What can patients expect from treatment with the iFuse Implant System?
Clinical studies have demonstrated that treatment with the iFuse Implant System improved pain, patient function, and quality of life.
What are the risks associated with the iFuse Implant System?
There are potential risks associated with the iFuse Implant System. It may not be appropriate for all patients and all patients may not benefit. For information about the risks, visit www.si-bone.com/risks.
What are the benefits of the iFuse Implant System?
The benefits of the iFuse Implant System include:
- It is a minimally invasive surgical approach.
- The triangular implant profile minimizes rotation and an interference fit minimizes micromotion.
- The porous surface promotes bony ongrowth and ingrowth.
- It is designed especially to stabilize and fuse the heavily loaded SI joint.
- The rigid titanium construction and implant geometry provide immediate stabilization.
What makes the iFuse Implants different from other fusion devices?
The iFuse ImplantsTM have a unique triangular shaped design to maintain their implant position over time. The implants allow for bony ongrowth and ingrowth and promote fusion of the SI joint over time.
What are the iFuse Implants made of?
The iFuse Implants are small titanium rods about the size of your little finger. Titanium is a very strong but lightweight material, commonly used for medical device implants.
What can you expect after SI joint fusion surgery with iFuse Implants?
At the time of discharge, Dr. Ball will provide post-surgical care instructions based on your medical health. He will also arrange for follow-up visits to assess your progress, the status of your incision, and your health status. You may experience some post-op buttock swelling, which can be alleviated by icing the region after surgery.
What is recovery like after SI joint fusion surgery with iFuse Implants?
After surgery, you will be partial weight-bearing for 3-4 weeks with the use of crutches or a walker. Dr. Ball will assess your progress and decide when you can return to full weight-bearing and resume your daily activities.
Can you have an MRI after receiving iFuse Implants?
A patient with this device can be scanned safely, immediately after placement, with some conditions. Dr. Ball can advise further on this issue.
Minimally Invasive Spine Surgery in San Ramon, California, and Fremont, California
If you are interested in scheduling a consultation with CalSpine MD for sacroiliac joint pain, please call (925) 667-3565. You may also Request An Appointment online.







